Vu Orthodontics - Orthodontics, Periodontics, and Implants
16027 Brookhurst St., Ste. K
Fountain Valley, CA 92708
ph: 714-775-0100
fax: 714-463-2205
drhungvu
- Home
- COVID-19 Notice
- CBCT
- CBCT & Chiropractic
- Biomechanics
- Services
- About Us
- Meet the Doctors
- Contact Us
- Cases
- Testimonials
- Emergency
- Office
- Ortho TADs
- Class II ("overbite")
- Class III ("underbite")
- Extremely Crowded
- Oral Surgery & Periodontics for GP
- Implants
- Medications
- Phlebotomy, PRF, PRP & SB
- Phase I (Pre-Teen Orthodontics)
- Adult Orthodontics
- Lasers
- Impacted Canines
- Accelerated Orthodontics
- Impacted Wisdom Teeth
- Referral Form
- Study Club
- Journal Articles
Wisdom Tooth
Impacted Wisdom Teeth: To save or not to save?
For Impacted Wisdom Teeth (IWT), the dilemma is to save or not to save? That is the question.
According to some study, about 85% of people have impacted lower wisdom teeth, whereas only about 16% of people have impacted upper wisdom teeth.
Just like anything else, either extreme position is unwise. Extracting all wisdom teeth blindly is bad whereas saving all wisdom teeth is equally poor.
If the wisdom teeth are not impacted and do not have any problems, then they must not be extracted (removed). But if the wisdom teeth are impacted, then 2 options are available to the patients:
Option 1: If the patients have multiple missing teeth, then the impacted teeth should be brought into the arch(es) in such a way that good alignment is achieved, by means of orthodontics.
Option 2: If the patients do not have multiple missing teeth and their jaws cannot accommodate all the teeth, then the impacted teeth should be removed.
Saving the Impacted Wisdom Tooth
The following example shows a case of an orthodontic patient that needs four premolars extracted. In this case, saving wisdom teeth is the right thing to do. Figure 1 shows an image of impacted wisdom tooth #17.

Fig. 1 Impacted wisdom tooth #17
Figure 2 shows the result of impacted wisdom tooth #17 corrected after orthodontic treatment.

Fig. 2 Wisdom tooth #17 corrected by orthodontics (near the end of the treatment)
Wisdom-Tooth Extraction Without Bone Grafting
The consequence of a typical extraction (removal) of a 3rd molar (wisdom tooth) is that the distal side of its adjacent 2nd molar has a bony defect.
An extraction is called typical here means an extraction without bone graft.
Another complication of a typical extraction of a wisdom tooth is a dry socket due to the loss of blood clot. A dry socket is accompanied by a severe pain because the nerves in the bone are exposed.
Figure 3 shows an example of the impacted lower left wisdom tooth (#17). The tooth is horizontally impacted and almost completely bony. The extraction was done without a bone graft. This type of bone graft is called socket graft. The result is, more than likely, that the lower left second molar (tooth #18) will suffer a bony defect on its distal side.

(a)

(b)

(c)
Fig. 3 Horizontally impacted lower left wisdom tooth (#17): (a) before extraction, (b) BW radiograph after extraction, without socket graft, (c) PA radiograph after extraction, without socket graft
Figure 4 shows an example of the impacted lower right wisdom tooth (#32). The tooth is horizontally impacted and almost completely bony. The extraction was done without the socket graft. The result is, more than likely, that there will be a bony defect on the distal side of the lower right second molar (tooth #31).

(a)

(b)

(c)
Fig. 4 Bony defect on the distal side of Tooth #31, after the wisdom tooth #32 is extracted without socket graft: (a) before extraction, (b) BW radiograph after extraction, (c) PA radiograph after extraction
For Impacted Wisdom Teeth, Doing Nothing is a Bad Option
For impacted wisdom teeth, especially on the lower, doing nothing is a bad option. Figure 5 shows the damages to the lower 2nd molars by the corresponding lower wisdom teeth.

(a)

(b)
Fig. 5 Damages to the lower 2nd molars by the wisdom teeth: (a) damaged lower right 2nd molar, (b) damaged lower left 2nd molar.
Another example of damages to the lower 2nd molars by the lower wisdom teeth is shown in Fig. 6.

(a)

(b)
Fig. 6 Damages to the lower 2nd molars (Teeth #31 & #18) by the wisdom teeth (Teeth #32 & #17): (a) panoramic radiograph, (b) Tooth #31 is the lower right 2nd molar; Tooth #18 is the lower left 2nd molar
Other Thoughts on Wisdom Teeth Extraction
A typical person has 32 teeth. In this writing, 3rd molars and wisdom teeth are used interchangeably.
For orthodontic treatment, if 4 premolars must be taken out, the person will have only 28 teeth. And if 4 wisdom teeth must be removed, then the person has only 24 teeth, after losing 8 teeth. That is a lot of teeth missing.
And later on in life, the person may lose more teeth due to disease or accident. The downside of having fewer teeth is two-fold: the jaws get smaller and the chewing power is significantly less.
Thus, for a patient who has 4 premolars missing, it would be beneficial to save the impacted wisdom teeth by uprighting and aligning them -- if they are healthy. The dentist must present this choice to the patient, and it is up to the patient to decide. Of course, uprighting the impacted 3rd molars will cost time and money.
On the other hand, if a person has all 32 good teeth but has no space for the impacted wisdom teeth, then extracting the problematic wisdom tooth/teeth is appropriate.
When a mandibular wisdom tooth is impacted and in contact with its adjacent 2nd molar, it almost always has granuloma which must be removed. If a wisdom tooth is impacted but causes no problem whatsoever (now or later), it is appropriate to leave it alone.
Some Different Opinions
The following link offers some opinion by the different author(s):
http://en.wikipedia.org/wiki/Wisdom_tooth
Although not everything written on Wikipedia is 100% accurate, it is a source for some readers. The following is its recommendation:
"In the U.K., the National Institute for Health and Clinical Excellence, which appraises the cost-effectiveness of treatments for the National Health Service, has argued that there is no evidence that removing disease-free impacted wisdom teeth is beneficial, and recommends against removal to avoid the various risks and discomforts of the procedure.[16]
The American Association of Oral and Maxillofacial Surgeons recommends that third molars be removed in patients who, in the opinion of their family dentists, suffer from periodontal infections where the probing depth exceeds 3 mm. It argues that it is advisable to have the third molars of such patients removed in young adulthood to avoid the complications that may occur when third molars have grown to maturity. In these cases, there is a greater likelihood of nerve damage and other potential concerns.[14]
The American Public Health Association recommends against prophylactic removal of asymptomatic, non-pathological wisdom teeth, including wisdom teeth that are impacted,[17] on the basis that the removal of third molars (wisdom teeth), like the removal of any teeth, should be based on evidence of diagnosed pathology or demonstrable need, rather than anticipated future pathology. The APHA's position is based on scientific research that documents the risks of injury to the nerves of the jaw that can cause permanent numbness of the lip and tongue, damage to the temporomandibular (jaw) joint and adjacent teeth."
Implant Dentistry and Missing Teeth (Especially Molars)
If a patient presents with a missing tooth, a bridge should no longer be a treatment choice in modern dentistry. For adults, implant dentistry is a good option.
But if there is inadequate space for a proper implant, an option is closing the space orthodontically.
For a missing 1st molar with adequate space, a viable option is moving the 2nd and 3rd molars forward, orthodontically, to close the space of the missing tooth. Of course, techniques of accelerated orthodontics should be utilized to shorten the treatment time.
An implant if done properly can last for a long time, perhaps 30 years, whereas a failed implant can occur in the following days or weeks after placement. According to some current study, the average lifespan of an implant is about 10 yrs.
Thus, if the infection can be treated, one should hang on to the natural healthy tooth as long as possible, and an implant would be the last option.
It is important to note that there is a huge difference between success and survival of an implant.
Wisdom-Tooth Extraction With Bone Grafting
If an extraction (removal) of a 3rd molar is accompanied by a successful bone graft, then its adjacent 2nd molar will not have a bony defect on the distal side. There will be no dry socket either because there will be no loss of blood clot and the bone will not be exposed.
Bone graft material can be an allograft or a xenograft (e.g., Bio-Oss) from a bone bank. But the best material is the biologic one from the patients themselves.
A tooth can be hopeless but certainly not useless. When the extracted tooth is used as a bone substitute, it is called dentin graft.
Although it is called dentin graft, all the hard substances of the tooth can be used: cementum, dentin, and enamel. A single-rooted tooth comprises a crown and a root. The crown is composed of enamel on the outside and dentin on the inside. The root comprises cementum on the outside and dentin on the inside. Inside the tooth lie the nerve and the blood vessels (vein and artery).
The dentin and cementum of the extracted tooth have many growth factors that promote bone healing and growth.
Although the enamel (of the extracted tooth) does not have any growth factor, it can work as a scaffolding for bone growth. Note that bone cells cannot grow directly on enamel. Thus, large chips of enamel must be discarded. Enamel, the hardest substance of the body, contains the highest percentage of minerals. And the main mineral is hydroxyapatite (a crystalline calcium phosphate).
As an example for this section, an impacted lower 3rd molar (lower wisdom tooth) is extracted, and dentin grafting is used.
The lower right wisdom tooth, #32, was impacted and had an occlusomesial decay. Since the patient had all 32 teeth, this tooth was decided to be extracted. The radiolucency underneath the crown of tooth #32 and distal to the crown of tooth #31 represents a granuloma (Fig. 7).
 (a)
(a)
(b)
Fig. 7 Lower right wisdom tooth, #32, with a decay (occlusomesial) and a granuloma (mesial): (a) bitewing (BW) radiograph, (b) photo, after extraction
A granuloma (also called inflammatory tissue) is a collection of inflammatory cells at the infection site. It includes activated macrophages and Langhans’ giant cells.
Note that granuloma is not the same as granulation tissue although some are confused and thought that the two terms could be used interchangeably.
Granulation tissue is the opposite of necrotic tissue or granuloma. Granulation tissue is healthy, normal, and desirable, whereas granuloma is infectious or inflammatory.
The English words granulating or granulated come from the Latin word granum, meaning "grain or seed." When the wound is healing, granulation tissue is formed. It is often lumpy or bumpy (hence the term, granulation). It has the color of light red or pink, coming from the many small blood vessels in the newly formed connective tissue.
The procedure is given as follows. First, the tooth is extracted (Fig. 7b)
Second, the tooth is mechanically cleaned by removing all carious lesions, granuloma and attached soft-tissues (Fig. 8). And the most effective way of removing the gross soft tissue is by using a scalpel. (If there were some calculus or a composite or amalgam filling, then it should be removed by a high-speed handpiece with a tungsten carbide.)
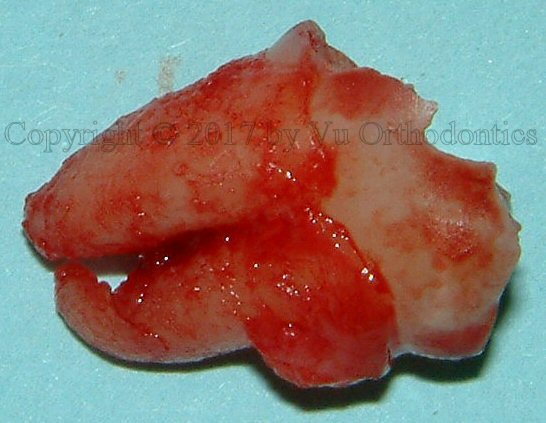
Fig. 8 Tooth #32, after mechanically cleaned, and one of the roots is sectioned
It must be emphasized that a tooth that has an RCT (root canal therapy) must not be used. The reason is that root canal sealers typically are zinc oxide-eugenol-based, calcium hydroxide-containing, glass-ionomer-based, epoxy-resin-based and methacrylate-resin-based sealers. And it is impossible to remove these chemicals from the root(s), including the dentinal tubules.
Third, the whole tooth (crown and roots) are placed in the Smart Dentin Grinder (KometaBio) for grinding (Fig. 9). Note that for teeth with well-separated roots, the roots must be severed before grinding; otherwise, the blades may get stuck in the roots and cannot turn. Then, the machine's motor would burn out.
Fig. 9 The grind chamber with the blades and the extracted tooth
Surprisingly, the machine has no difficulty in grinding the enamel of the crown.
Dentin grafting is not free because the cost includes the grinding chamber and the time to process it. But dentin grafting is great for bone growth because it has slow-releasing growth factors. It is also the patient's own biologic material.
The settings for the grinding is 3 s and 20 s for the grinding and sorting, respectively. As the machine grinds, the tooth particulates pass through the floor of the grind chamber.
Next, the particulates with the proper sizes are collected by the tray (drawer) and then placed on a dish (Fig. 10). The floor has larger holes that allow only particulates that are smaller than 1200 microns pass through. And the tray has a sieve with smaller openings that allow only particles that are smaller than 250 microns going through. Thus, the collected particulates range from 250 to 1200 microns (or 0.250 to 1.2 mm). Again, in dentin grafting, tiny particulates of enamel can be included, but large chips of enamel should be discarded since bone cells cannot grow on enamel.
Fig. 10 The tooth particulates (a mixture of dentin, cementum, and enamel) but so-called "dentin graft"
According to Dr. Izhak Binderman, with any grafts that are smaller than 50 microns, the macrophages will engulf them and become giant cells. Then, the inflammatory phase is prolonged. On the other hand, there is no harm having a few pieces of enamel, even up to around 2000 microns (2 mm). They are just hydroxyapatite.
Fourth, the particulates are then chemically cleaned by Dentin Cleanser (Fig. 11) which a highly alkaline liquid for about 10 minutes to dissolve the organic materials, yielding inorganic minerals.
Fig. 11 Dentin Cleanser and phosphate-buffered saline
Fifth, phosphate-buffered saline (PBS), also shown in Fig. 9, is used for about 3 minutes (to neutralize the cleanser). PBS is a water-based salt solution containing disodium hydrogen phosphate, sodium chloride and, in some formulations, potassium chloride, and potassium dihydrogen phosphate. The buffer helps to maintain a constant pH.
Finally, the particulates can be mixed with PRF (platelet-rich fibrin) to make Sticky Bone (the bone that is sticky), ready for grafting the extracted site. PRF has many growth factors that enhance healing. And the handling of the grafting material is much easier with Sticky Bone, especially when the grafting site is bleeding. Examples of PRF and Sticky Bone are shown in Fig. 12 and Fig. 13, respectively.
Fig. 12 An example of PRF
Fig. 13 An example of Sticky Bone
One or two (2) layers of PRF can be placed on top of the grafting material to act as the barrier membrane. There would be no need to use any collagen membrane in addition to the PRF membrane. In the end, the surgical site was then sutured with tension free.
As a side note for dental implants (in the site other than wisdom teeth), one must not try to get a primary closure. It is better to let the healing done by secondary intention. Doing so would yield more keratinized mucosa for the site. And, typically, the grafted site will be ready for implant placement after approximately 4 months for the mandible and 6 months for the maxilla (since the bone in the maxilla is less dense).
Afterward, a BW radiograph was taken (Fig. 14).

Fig. 14 The tooth was ground, processed, mixed with PRF, then grafted to the extraction site.
The beauty of this application is the grafting material is the patient's own (with all the growth factors included), instead of using processed material from a cadaver or an animal (e.g., cow, pig, horse). In addition, there is no cost of purchasing the grafting materials, including the collagen membranes.
The question arises is do we need to use a collagen membrane when we already have PRF? The answer is it may be unnecessary or even counterproductive. From a limited clinical observation, when a collagen membrane (e.g. BioXclude) was used on top of the PRF membrane, the clinical outcome was not as good as expected. It is a possibility that the PRF may adversely interact with the collagen membrane.
Note that PRF is not just a membrane, it is alive with all active cells (neutrophils, lymphocytes, monocytes, eosinophils, basophils, and platelets).
It is unanimously agreed by many health professionals that PRF helps with soft tissue healing. Currently, the debate is still on: if PRF and PRP help bone growth.
Notice that in many cases of typical extractions of mandibular 3rd molar, its adjacent 2nd molar suffers a bony defect on the distal site. Another complication is a dry socket (with severe pain) where the bone with nerve endings is exposed due to the loss of blood clot.
In summary, when a mandibular wisdom tooth is impacted and in contact with its adjacent 2nd molar, the associated granuloma must be removed. And if the extraction site is grafted properly, the 2nd molar will not suffer the bony defect on its distal site nor the dry socket.
© Copyright 2007-2014, Vu Orthodontics. All rights reserved.
Serving communities: Orange County, Fountain Valley, Huntington Beach, Westminster, Garden Grove, Anaheim, Santa Ana, Buena Park, Tustin, Costa Mesa, Newport Beach, Irvine, Stanton, Cypress, Seal Beach, Los Alamitos, Fullerton, La Habra, Brea, Yorba Linda, Placentia, Villa Park, Lake Forest, Mission Viejo, Laguna Beach, Laguna Niguel, Laguna Hills; Los Angeles, Long Beach...
16027 Brookhurst St., Ste. K
Fountain Valley, CA 92708
ph: 714-775-0100
fax: 714-463-2205
drhungvu